Table of Contents
The activated partial thromboplastin time (APTT or aPTT) is a coagulation test used to evaluate low-dose heparin therapy and test for the function of hemostasis’ intrinsic and normal pathway. The reagent used to perform the APTT is partial thromboplastin, which is the lipid portion of thromboplastin in the tissue. The partial thromboplastin reagent is manufactured from rabbit or bovine brain tissue as well as food ingredients such as soybeans. In the APTT test, partial thromboplastin performs the platelet factor 3 (PF3) function.
The APTT is so called because the partial thromboplastin reagent used in the analysis contains activators like Kaolin or Silica that stimulate the intrinsic pathway clotting factors. The second reagent used in the analysis is calcium chloride (CaCl2), which provides the ionized calcium needed to activate prothrombin in the typical pathway.
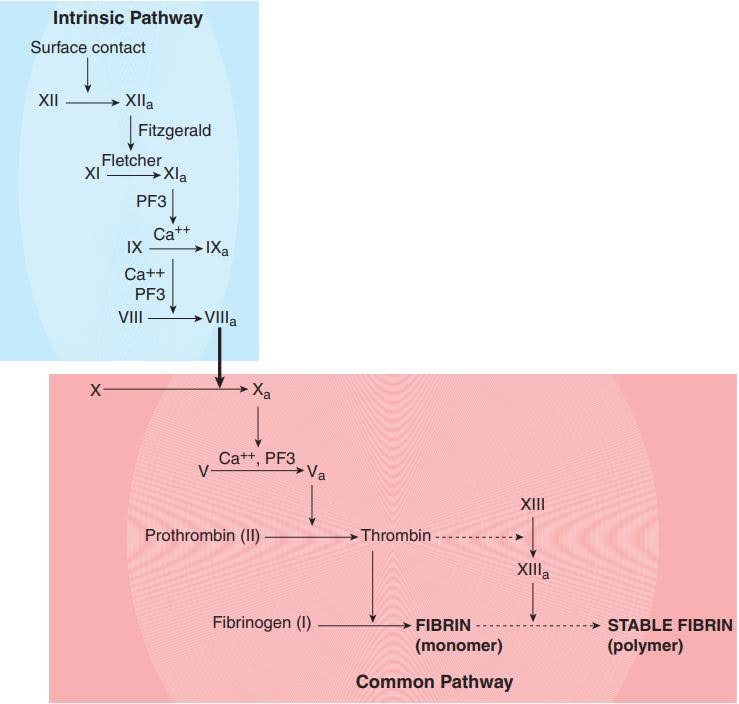
The phospholipid (PL), a negatively charged particulate activator (NCS), and ionized calcium comprise the partial thromboplastin reagent (PTT). It activates the intrinsic and specific pathways of the coagulation system through the contact factors XII, prekallikrein (Pre-K; also known as Fletcher factor), and high-molecular-weight kininogen (HMWK; also known as Fitzgerald factor), none of which are involved in the in vivo coagulation process. Deficiencies in Pre-K, HMWK, factors XII, XI, IX, VIII, X, and prothrombin, as well as fibrinogen when fibrinogen levels are less than 100 mg/dL, prolong the PTT.
The defects for which the PTT reagent is specifically calibrated are factors VIII, IX, and XI. Since heparin inhibits plasma antithrombin, which neutralizes all plasma serine proteases, including thrombin (IIa) and active factor X, the PTT is prolonged during heparin therapy (Xa). The PTT is prolonged in the presence of lupus anticoagulant since the anticoagulant neutralizes essential phospholipids in reagents. The PTT does not find a defect in factor XIII. TF, Tissue factor; Pro, prothrombin (II, zymogen); Wr, thrombin (activated factor II, or IIa; serine protease); Va, VIIIa, activated factor V and VIII (serine protease cofactors); VIIa, IXa, Xa, XIa, activated factor VII, IX , X, XI (serine proteases); XIIa, activated factor XII (serine protease but not part of in vivo coagulation); XIIIa, activated factor XIII (transglutaminase).
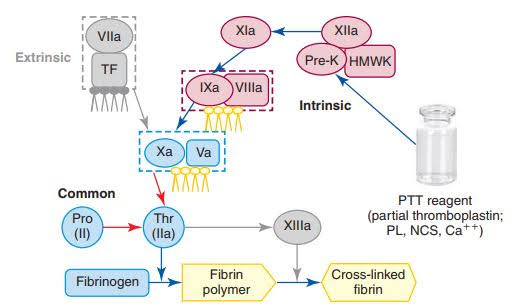
The factors XI, IX, VIII, X, and V; prothrombin; and fibrinogen when fibrinogen is 100 mg/dL or less are the factors whose deficiencies are consistent with hemorrhage and are expressed in sustained PTT studies, in order of reaction. If the PPP test has less than around 0.3 units / mL (30 percent of normal) of VIII, IX, or XI, most PTT reagents are designed to prolong PTT. PTT is also prolonged by anti-factor VIII antibodies, factor IX antibodies, and other coagulation factors, as well as therapeutic heptic agents, in the presence of LA, an immunoglobulin with phospholipid-bound protein affinity. Factor VII and factor XIII deficiency have no effect on the PTT. Factor XII, prekallikrein, and high-molecular-weight kininogen deficiencies prolong the PTT but do not result in bleeding.
Partial Thromboplastin Time Test
Reagent
Reagent consisting of phospholipid and particulate activator cephaloplastin (phospholipid preparation) obtained from the rabbit brain with ellagic acid as an activator reagent for evaluating the active partial thromboplastin time.
Principle
Cephaloplastin acts in the presence of calcium ions, the coagulation agents in the intrinsic pathway of the coagulation system. APTT is exacerbated by a loss of one or more of these underlying channel clotting factors and in the presence of coagulation; such as heparin inhibitors.
Sample Collection and Preparation
No special patient preparedness is required by approved techniques prior to sample collection. The venipuncture needs to be a ‘clean’ without excessive venous stasis. Once the needle is removed from the syringe, transfer the blood into tubes. Mix with one part of Trisodium citrate exactly nine parts of the freshly collected blood (0.11 mol / L, 3.2 percent). Immediately centrifuge at 3000 rpm (about 2000 g) for 15 minutes, then move the plasma into a sterile test tube. Plasma has to be checked within three hours of collecting the blood. Platelet deficient plasma should be used for determination of heparin, hence higher centrifugation time is required.
Partial Thromboplastin Time Reference Interval
The PTT comparison period varies by patient group, reagent size, instrument size, pH, and diluent purity. The reference period for a laboratory at the medical center is set at 26 to 38 seconds. Its crucial each laboratory set its own normal PTT for each new lot of reagent. This can be achieved by analyzing a selection of 30 or more specimens from healthy donors of both sexes covering the adult age spectrum for several days and measuring the 95 percent confidence interval of the findings.
Clinical Implications of APTT
- The APTT is prolonged in all coagulation defects of stage I (includes platelet activity and thromboplastin).
- The APTT is usually prolonged in Willebrand’s disease and is accompanied by a consistently diminished factor VIII level.
- The APTT and PT will detect 95% of coagulation abnormalities. When APTT is performed in conjunction with a prothrombin time (PT), a further clarification of coagulation defects is possible. For example, a normal PT and abnormal APTT means that the defect lies in the first stage of the clotting mechanism.
Causes of prolonged APTT
- Hemophilia
- Vitamin K deficiency
- Liver disease
- Presence of circulating anticoagulants
- DIC disease (chronic or acute).
Shortened APTT occurs in:
- Extensive cancer, except when liver is involved
- Immediately after acute hemorrhage
- Very early stages of DIC.
References:
- Rodak’s Hematology 5th Edition, Elsevier.
- Basic Clinical Laboratory Techniques 6th Edition, Delmar Cengage Learning
- Concise Book of Medical Laboratory Technology 2nd Edition, Jaypee
