Table of Contents
All of the stable materials suspended in the urine are referred to as “urine sediment.” Microscopic analysis of urine sediment is useful to rule out kidney and urinary tract disease. Microscopic examination of such observations can contribute to the interpretation of faulty physical and chemical tests. The epithelium, liver, lower genitourinary tract, and external contaminants all contribute to the accumulation of components in urine.
The substances accumulated include RBCs, WBCs, epithelial cells, casts, bacteria, yeast, fungi, mucus, crystals, spermatozoa. Because some of these elements have no clinical significance and some are considered normal unless found in excessive quantities, a urine sediment study must give both identification and quantification of the components present.
Preparation of the Urine Sediment
A standard volume of urine, often between 10 and 15 mL, is centrifuged in a conical tube. It provides you with the optimum amount of content to obtain a representative sample of the components in the sample.
The duration of time the specimen is centrifuged is related to the speed of the centrifuge. A five-minute centrifugal force (RCF) of 400 produces the best amount of sediment that is less likely to destroy the constituents.
Until decantation, a standardized volume of urine and sediment will remain in the tube. Volumes of 0.5 to 1.0 mL are normally employed. The concentration factor is calculated by dividing the number of sediments by the amount of urine centrifuged. The sediment concentration factor is used to calculate the amount of elements present per mililiter, which relates to the likelihood of recognizing elements present in low quantities.
Volume of Sediment Examined
Each specimen’s sediment volume on the microscope slide should be consistent. The recommended volume for the traditional glass-slide technique is 20 μL (0.02 mL) filled with a 22 x 22 mm glass cover slip. If the specimen is allowed to flow outside of the cover slip, heavier components such as casts will be lost.
Analysis of Urine Sediment
It is necessary to distinguish both common and rare constituents in order to evaluate. Normal constituents are usually more noticeable under the microscope, and they must be marked so that the existence of the less observable but more important abnormal constituents is not masked. The microscopic examination can be carried out consistently, with at least 10 fields examined at low (10x) and high (40x) power levels. The slide is examined under low power first to locate casts and assess the overall composition of the material. As elements like casts are identified, the magnificaton is increased to high power.
Low-Power Examination
Look for the following with the low-power (x10) objective:
- Casts. Inspect the entire area for the existence of casts using uniform slides. Look for casts around the four corners of the coverslip , then in the centre for slides.
- When you find a cast, switch to high power to identify it.
- Casts are graded and reported based on the total number of casts seen per low-power field. If a single specimen contains more than one type of cast, classify and grade each type separately.
- Amorphous and crystals are examined in the same way that you can look for casts.
- If normal crystals are present, they are reported as few, moderate, or many per high-power area. Crystals, on the other hand, can be more visible at LPF.
- When abnormal crystals are present, they are reported based on the average amount seen per LPF. Until abnormal crystals are identified, they must be verified by a chemical test or a patients clinical history.
- Crystals are identified by their shape rather than their size. As a result, identification need a mix of low- and high-power observations.
- Epithelial cells (squamous epithelium): Report as few, mild, or many per LPF if present.
- Mucus (mucous threads): When easily seen or prominent under low power, these are reported as current. Phase-contrast microscopy makes them more visible.
High-Power Examination
With high-power (×40) objective, search for the following:
- Red blood cells. The average amount of RBCs seen per high-power is used to grade and evaluate. If some irregular shapes, such as dysmorphic red cells, are seen report them.
- White blood cells. Commonly, they are neutrophils (PMNs). Report any rare cell forms, such as lymphocytes or eosinophils, that are morphologically recognizable.
- Normal crystals. Each type of crystal observed should be identified and reported as few, small, or many per high-power region.
- Casts. Use high power to identify, but low power to grade.
- Epithelial cells: Renal tubular, oval fat bodies (renal tubular cells with fat), and transitional. Estimate and record as few, moderate, or many per high-power sector where these are present.
- Miscellaneous. This group contains yeast, bacteria, trichomonads, and fat globules, as well as other cell types and other structures found in urine sediment. Where these are present, classify the cell or structure and record the number of cells or structures per high-power field as few, moderate, or more. Just report the presence of sperm in males. It is not recorded in normal urinalysis specimens from females because it is considered a contaminant.
The content of urine sediments
The major portion of urine fluid is composed of biological or chemical elements. RBCs (erythrocytes), WBCs (leukocytes), epithelial cells, organic fat, casts, bacteria, yeast, fungus, parasites, and spermatozoa are all present in the biological section of the sediment. (The casts are lengthy cylindrical objects that develop as the fluid within the kidney tubule lumen freezes.) More kidney disease or disorder, tumors, tumor or lesion, stone development, and frequent bleeding disorders, as well as the use of anticoagulants, are all biological components.
Hematuria is a significant early sign of renal disease. Chemical crystals and amorphous material make up the chemical component. It is, on average, less important than that section of biology. However, numerous rare crystals have pathogenic consequences. Furthermore, the components of a crystalline or chemical substance are sometimes so diverse that they appear to hide the most vital parts, which must be carefully investigated.
Several Urinary Crystals are described below.
| Crystal | pH | Color | Solubility |
| Uric Acid | Acid | Yellow-Brown | Aklali Soluble |
| Amorphous Urates | Acid | Brick Dust or Yellow | Alkali and heat |
| Calcium Oxalate | Acid/Neutral | Colorless | Oval on Dilute HCL |
| Amorphous Phosphates | Alkaline/Neutral | White-Colorless | Dilute acetic acid |
| Calcium Phosphate | Alkaline/Neutral | Colorless | Dilute Acetic acid |
| Triple Phosphate | Alkaline | Colorless | Dilute Acetic acid |
| Ammonium Biurate | Alkaline | Yellow-Brown | Acetic acid with heat |
| Calcium carbonate | Alkaline | Colorless | Gas from acetic acid |
| Cystine | Acid | Colorless | Ammonia, Dilute HCL |
| Cholesterol | Acid | Colorless | Chloroform |
| Leucine | Acid/Neutral | Yellow | Hot alkali or alcohol |
| Tyrosine | Acid/Neutral | Colorless-Yellow | Alkali or Heat |
| Bilirubin | Acid | Yellow | Acetic acid, HCl, Naoh |
| Sulfonamides | Acid/Neutral | Varied | Acetone |
| Radiographic dye | Acid | Colorless | 10% NaoH |
| Ampicillin | Acid/Neutral | Colorless | Refrigeration forms |
Images of frequently found urine sediments







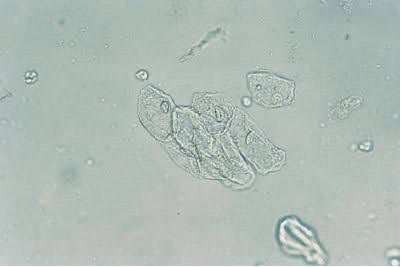

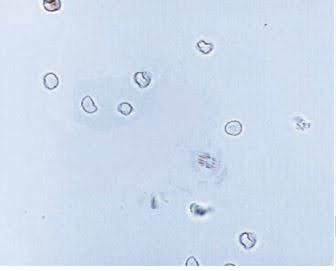



References:
- Strasinger, S. K., & Di, L. M. S. (2014). Urinalysis and body fluids. Philadelphia: F.A. Davis Co.

very good pictures