Table of Contents
Magnesium testing is an essential component of clinical laboratory evaluation, particularly in the assessment of electrolyte balance, neuromuscular function, and metabolic stability. Magnesium is the second most abundant intracellular cation and plays a critical role in over 300 enzymatic reactions, including ATP metabolism, DNA synthesis, and neuromuscular conduction. Despite its physiological importance, magnesium disorders are frequently underdiagnosed due to subtle clinical manifestations and limitations in routine testing methods.
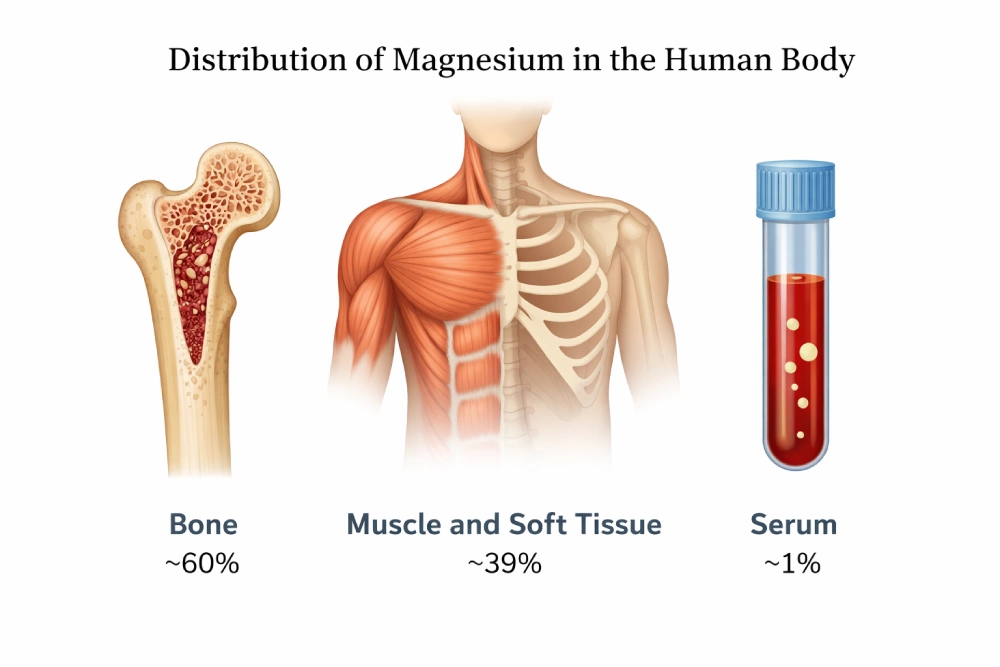
Clinically, magnesium testing is most often performed using serum magnesium measurement, but this represents only about 1% of total body magnesium, which can limit its diagnostic accuracy. Consequently, advanced testing methods such as ionized magnesium, intracellular magnesium assays, and magnesium loading tests are increasingly considered in complex cases. Magnesium imbalance—hypomagnesemia or hypermagnesemia—can have significant clinical consequences, including cardiac arrhythmias, neuromuscular dysfunction, seizures, and altered mental status.
Magnesium testing is particularly relevant in critically ill patients, individuals with chronic kidney disease, gastrointestinal disorders, diabetes mellitus, and those receiving medications such as diuretics or proton pump inhibitors. In intensive care settings, magnesium monitoring guides electrolyte correction and influences outcomes in patients with arrhythmias or sepsis.
Deficiency or excess can cause:
Principle of Magnesium Testing
Magnesium testing is based on the quantification of magnesium ions (Mg²⁺) in biological fluids, most commonly serum or plasma. Most routine assays rely on colorimetric or spectrophotometric detection.
Biochemical Basis
Magnesium is essential for:
- ATP-dependent enzymatic reactions
- Neuromuscular transmission
- Regulation of calcium and potassium channels
- Hormonal regulation including parathyroid hormone
Because magnesium is primarily intracellular, serum levels may not reflect total body stores.
Analytical Methods
- Colorimetric assays: Use dyes such as xylidyl blue or calmagite
- Atomic absorption spectrophotometry (AAS): Reference method with high specificity
- Ion-selective electrodes (ISE): Measure ionized magnesium
- Enzymatic assays: Indirect measurement via enzyme activity
Laboratory Procedure
Specimen Collection
- Sample: Serum or heparinized plasma
- Volume: 1–2 mL
- Avoid hemolysis and prolonged tourniquet use
Sample Handling
- Centrifuge within 30 minutes
- Store at 2–8°C if delayed
- Avoid EDTA or citrate tubes
Colorimetric Method Procedure
- Add reagent containing chromogen
- Mix with serum sample
- Incubate 5–10 minutes
- Measure absorbance at 520–550 nm
- Compare with standard calibration
Quality Control
- Run controls daily
- Maintain CV <5%
- Regular instrument calibration
Reference Range
- Adults: 1.7–2.4 mg/dL
Clinical Significance
Hypomagnesemia
Causes:
- Diuretics
- Alcoholism
- Malabsorption
- Diabetes
Symptoms:
- Arrhythmias
- Seizures
- Neuromuscular irritability
Hypermagnesemia
Causes:
- Renal failure
- Excess magnesium intake
Symptoms:
- Hypotension
- Bradycardia
- Respiratory depression
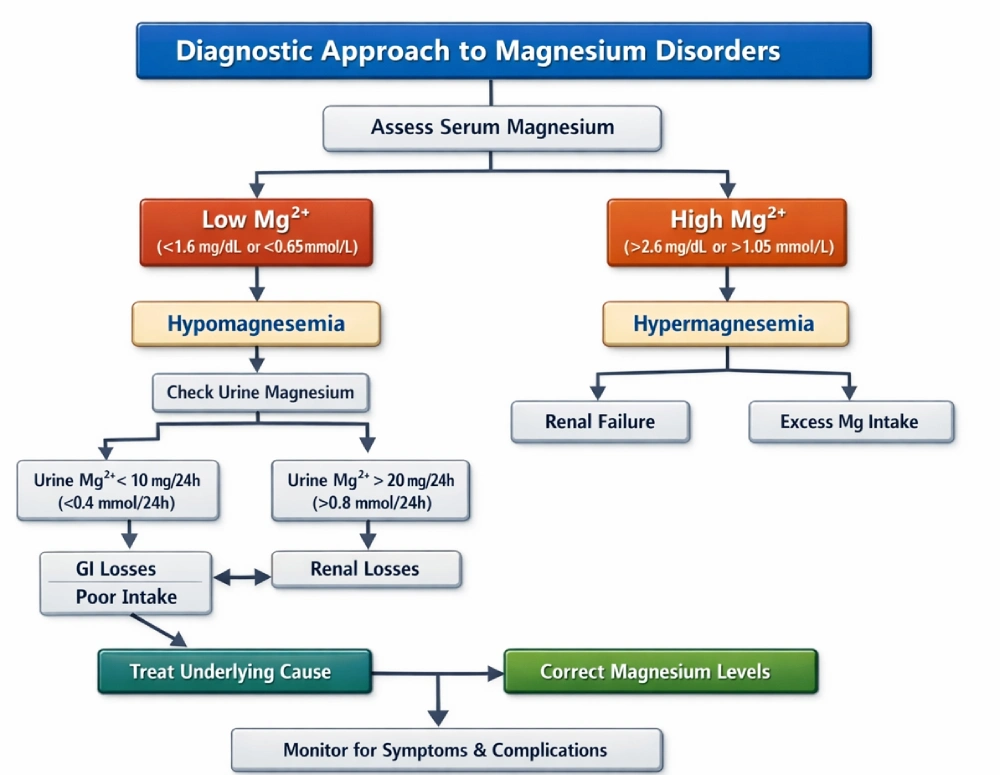
Interpretation of Results
| Result | Interpretation | Action |
|---|---|---|
| <1.7 mg/dL | Hypomagnesemia | Supplement magnesium |
| 1.7–2.4 mg/dL | Normal | Clinical correlation |
| >2.4 mg/dL | Hypermagnesemia | Identify cause |
Limitations
- Serum magnesium reflects only 1% of body stores
- Hemolysis causes false elevation
- Low sensitivity for chronic deficiency
- Interference from lipemia and bilirubin
Precautions
Laboratory
- Avoid hemolyzed samples
- Use correct anticoagulants
- Calibrate instruments regularly
Patient Care
- Monitor high-risk patients
- Consider repeated testing if clinically indicated
Conclusion
Magnesium testing remains a critical yet often underestimated diagnostic tool in clinical medicine. While serum magnesium measurement is widely accessible and useful for initial screening, its limitations require careful interpretation alongside clinical findings and additional laboratory parameters. Advanced methods such as ionized magnesium measurement provide more accurate assessment in critically ill patients.
References
- Burtis, C. A., & Bruns, D. E. (2019). Tietz Fundamentals of Clinical Chemistry. Elsevier.
- McPherson, R. A., & Pincus, M. R. (2022). Henry’s Clinical Diagnosis. Elsevier.
- Rifai, N. et al. (2018). Tietz Textbook of Clinical Chemistry. Elsevier.
- Elin, R. J. (2010). Assessment of magnesium status. Clinical Chemistry.
- Jahnen-Dechent, W., & Ketteler, M. (2012). Magnesium basics. Clinical Kidney Journal.
